Learn more about the process of spotting symptoms and understanding what Prostate Cancer involves
If you’ve just been diagnosed with prostate cancer, it can be a scary time, not only for you but for your loved ones as well. Here at Tackle, there are plenty of ways we can help you overcome the struggles you face.
Here we’ll guide you through the stages of diagnosis. Please bear in mind that this will be specific to you and your prostate cancer.
PSA, is produced by healthy cells in the prostate, so it’s normal to have a small amount in your blood. However, too much could create a cause for concern.
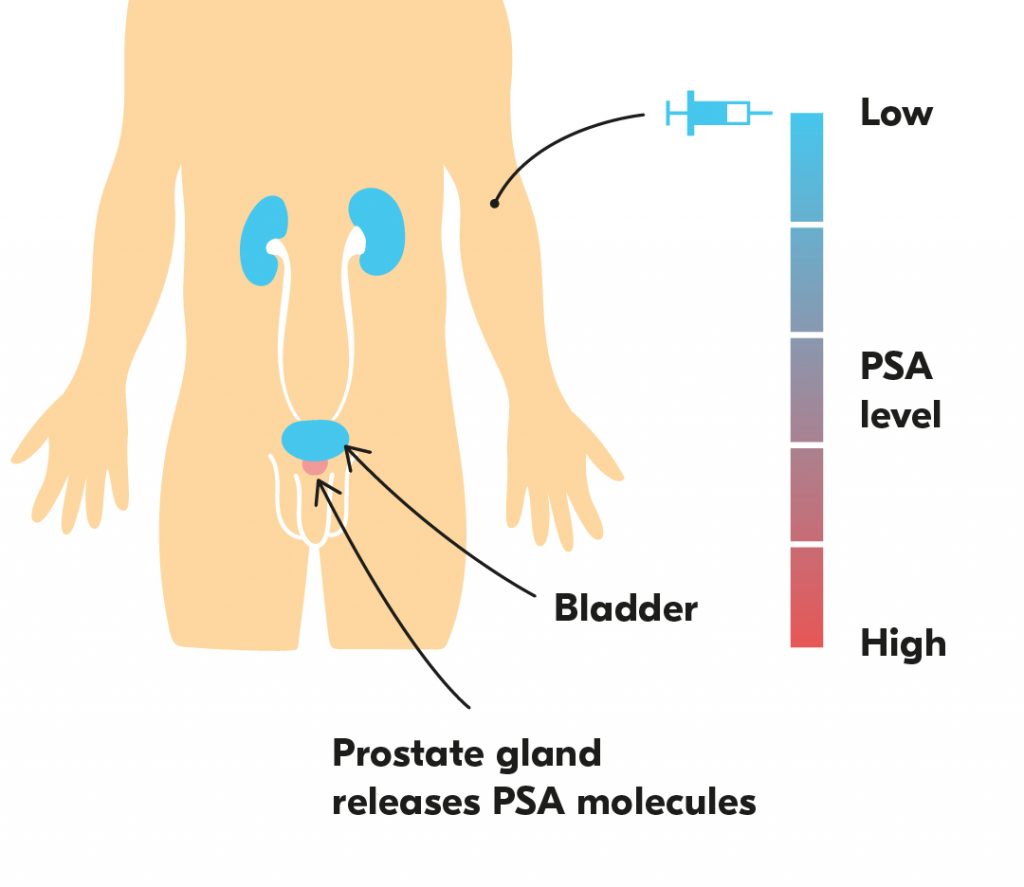
An initial PSA (whether planned, by chance or because of raised awareness) is important to have whether you have symptoms or not. It’s also important that you get this carried out at an appropriate time.
More info on when you should get your PSA done here.
Your healthcare professional will advise you on the next steps once you’ve had your PSA test. They might refer you to a specialist if they feel your PSA is higher than it should be, or if they think you’re at risk of prostate cancer due to having increased risk factors. They could also think that something else has caused your PSA level to be raised, so they might suggest having another PSA test in the future to see if your PSA level changes, rather than seeing a specialist straight away.
You should see a specialist within two weeks, this is sometimes called a ‘two-week wait’ or ‘fast-track’ referral.
A DRE is used to see if you have a prostate problem or prostate cancer. This will involve your healthcare professional feeling your prostate through the wall of your back passage (rectum). This is as important as your PSA, they’re not feeling how large it is more how it feels.
If you’re worried or feeling embarrassed about the DRE, do talk with the people at one of our support groups.
A multi-parametric MRI scan is a special type of scan that looks inside your prostate and assesses the size and position of relatively small tumours. It uses four different types of images which give a clearer idea as to whether there is cancer inside your prostate.
The MP MRI improves the accuracy when taking biopsy samples and avoids men having biopsies unnecessarily, as the scan only picks up cancers that are harmful and need further tests.
A prostate biopsy is where a thin needle takes small samples of tissue from the prostate, which is then looked at under a microscope to check for cancer. The results from this will show how likely it is to spread outside of the prostate and what can be done to treat it.
There are three main prostate biopsies, however other possibilities could be suggested depending on your circumstance:
This is to see if the prostate cancer has spread to the bones, which is a common place for the prostate cancer to spread to.
Let your healthcare specialist know if you have arthritis or have had any broken bones or surgery to the bones, as these will show up on the scan.
A small amount of dye is injected into the vein of your arm and travels around the body. If there is any cancer in the bones, the dye will collect in the areas and show up in the scan. This normally takes 2 – 4 hours. The areas where the dye has collected, are often called ‘hot spots’ and you may have to have an x-ray to see if these are cancerous.
The dye used for bone scans are safe, but radioactive. So you should avoid close contact with children and pregnant women for up to 24 hours after the scan.
This is often used to see if prostate cancer has come back after treatment, rather than when you are first diagnosed. A PET scan is normally combined with a CT scan (PET-CT) to give even more detail about any prostate cancer inside the body. The scan can detect very small areas of cancer.
When you first get your test results after just being diagnosed with prostate cancer, it can be a bit of a minefield and information can become confusing. If you’re unclear on anything, do ask your healthcare professional. Or, if possible take a loved one with you, so you have another pair of ears in the room.
Once you’ve had our scans, these will determine how far your cancer has spread and what treatments can be implemented. Below are the different types of prostate cancer:
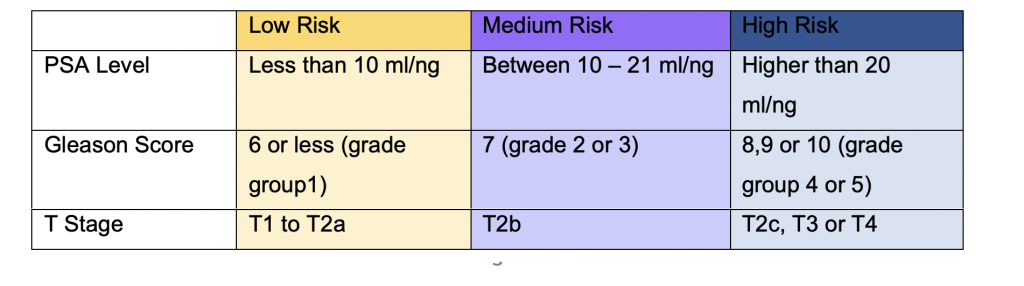
In order to find out how likely it is that your cancer will spread, your doctor will look at:
Grading can also be done with the ISUP score which is thought to be more explanatory that the Gleason score but not widely used in UK yet.
The current system of staging prostate cancer is known as the TNM system (standing for ‘Tumour/Nodes/Metastasis’).
T Stage: The T stage of the disease refers to the form of the primary tumour in the prostate. This shows how far the cancer has spread in and around the prostate. A DRE, MRI or sometimes a CT scan is used.
N Stage: refers to the pelvic lymph nodes near the prostate. It is rated from 0 to 3,
depending on the presence and extent of the spread.
M Stage: refers to the metastasis, i.e. the degree to which the prostate cancer has
travelled out of the immediate area of the prostate to other organs of the body.
For more detailed information please see here.
All your results will be discussed by the multidisciplinary team. MDT: definition. Where surgeon, oncologist, radiographer and specialist nurses will review all of your results and decide what’s appropriate for you.
Once you’ve had your initial diagnosis, it’s important to assess your treatment options to see which is right for you. If you’re unsure about anything to do with your treatment, then speak with your doctor, nurse or other healthcare professional to ensure you know what to expect pre, during and post treatment. They can also make sure you have the right steps in place through your treatment. It’s also useful to speak with someone who has been through the treatment(s) you are being offered. Speak with your local support group.
When you’re first diagnosed with prostate cancer, it can often send your mind into a spin and conversations can soon become a blur. It’s here we advise people, to take all the time you need to digest and process the news and read through any information provided from your doctor or GP.
If you can, take someone with you to your appointment, so you’ve got a second pair of ears to process the information and remember what has been said.
We have some information booklets you can read in your own time.
Every person is different. Which means everyone’s prostate cancer journey is different. There is no right or wrong way to feel at any stage of your prostate cancer journey and we’re not here to tell you otherwise.
We’re here to encourage you to talk about how you’re feeling and avoid suppressing or internalising any thoughts you may have. Whether it’s speaking with a friend or family member, or going to one of our friendly support groups.
There are people here to help that you’re not on this journey alone.
When your body is tackling prostate cancer, it’s essential to make it as fit and healthy as possible to ensure it’s in its best possible state to overcome any hurdles it needs to. Make sure your diet is rich in fruits and vegetables, and is balanced with fibre, carbohydrates, healthy fats and protein. We also recommend doing regular exercise and keep as active as you can throughout your prostate cancer journey.
Tackle Tip! Why not see if your local area has a walking or cycling group you could join? Many local support groups organise their own exercise classes, walks or coffee mornings. They can be a good way of talking closely with someone in a relaxed atmosphere.
Connecting with people who have been on or are going through their own prostate cancer journey, can provide an invaluable network of support. Any topics you may find embarrassing, upsetting or shameful, to discuss with your loved ones can be shared at one of our support groups. We have over 90 groups in the UK, where each are tailored to the individuals who are on their prostate cancer journey.
We’ve curated a collection of resources to help you learn more about Prostate Cancer and what you can expect through the process from diagnosis to treatment and beyond.

Learning to live with with the effects of Prostate Cancer doesn’t have to be difficult with our help and advice

There are over 150 prostate cancer support groups across the UK. Different places, different styles – all exist, to help you make sense of the complexities of prostate cancer.
Have another query? A member of our team are always here to help you and your loved ones with any questions you have regarding your prostate cancer.
Sign-up to our monthly newsletter for content about Tackle and Prostate Cancer that’s tailored to you.